Reproductive System
Table of Contents
The reproductive system, also called the genital system, is a collection of internal and external organs in both males and females that work together for the purpose of procreation. Its primary functions are to produce and store gametes (sex cells – sperm and egg), facilitate their union during fertilization, support the development of a new life and deliver it into the world.
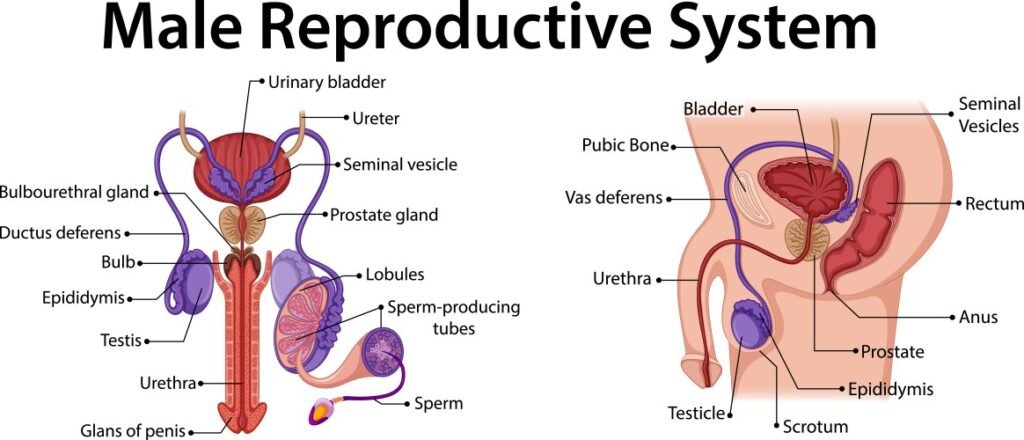
The male reproductive system is composed of both external and internal organs that function together to produce and deliver sperm for fertilization.
External Genital Organs
The external male reproductive organs are those that are visible outside the body. They include:
Penis: The penis is a cylindrical organ that serves a dual function:
Reproductive Role: It delivers semen, containing sperm, into the female reproductive tract during sexual intercourse. During sexual arousal, increased blood flow to the erectile tissue within the penis causes it to become stiff and erect, facilitating penetration.
Urinary Role: It contains the urethra, which serves as a conduit for both urine and semen. However, during ejaculation, a sphincter at the base of the bladder closes, preventing urine from mixing with semen.
Foreskin (Prepuce): A retractable fold of skin that covers and protects the glans penis (the sensitive head of the penis).
Smegma: A naturally occurring white, creamy substance produced by the penis, which helps the foreskin slide back smoothly. Accumulation of smegma under the foreskin can lead to odor or infection, so regular cleaning is important for uncircumcised men.
Scrotum: A sac-like structure made of skin and muscle that hangs behind the penis and between the thighs.
Function: Contains and protects the testes. It also plays a crucial role in regulating the temperature of the testes, which is essential for sperm production.
Testes (Testicles): Two oval-shaped organs located within the scrotum.
Functions:
Sperm Production: The primary site of sperm production (spermatogenesis).
Hormone Production: Produce testosterone, the primary male sex hormone responsible for the development of male secondary sexual characteristics (e.g., deepening of the voice, increased muscle mass, facial hair growth).
Internal Reproductive Organs
The internal male reproductive organs are located within the body and are responsible for sperm maturation, transport, and the production of seminal fluid.
Epididymis: A pair of long, tightly coiled tubes located on the top and back of each testis.
Functions:
Sperm Storage: Stores sperm as they mature.
Sperm Maturation: Sperm complete their maturation process within the epididymis, gaining motility (the ability to swim).
Vas Deferens (Deferent Ducts): Two muscular tubes that transport mature sperm from each epididymis to the ejaculatory ducts.
Seminal Vesicles: Two small, pouch-like glands located behind the bladder.
Function: Produce a significant portion of the fluid that makes up semen. This fluid is:
Alkaline: Helps neutralize the acidity of the female reproductive tract, increasing sperm survival.
Rich in Fructose: Provides energy for sperm motility.
Important Note: The seminal vesicles do not store sperm.
Ejaculatory Ducts: Short ducts formed by the union of the vas deferens and the duct of the seminal vesicle. They pass through the prostate gland and empty into the urethra.
Prostate Gland: A walnut-sized gland located just below the bladder and surrounding the urethra.
Function: Secretes a milky, slightly alkaline fluid that contributes to semen volume and helps with sperm motility and viability.
Bulbourethral Glands (Cowper’s Glands): Two small, pea-sized glands located below the prostate gland on either side of the urethra.
Function: Secrete a clear, viscous fluid (pre-ejaculate) that lubricates the urethra and neutralizes any residual acidity from urine.
Urethra: A tube that extends from the bladder through the prostate gland and the penis to the outside of the body. It serves as a common pathway for both urine and semen (though not simultaneously).
Arterial Supply, Venous Drainage, and Nervous Supply of the Male Reproductive System
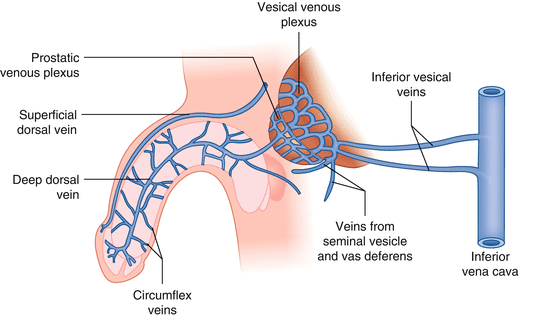
Arterial Supply: The primary arteries supplying blood to the male reproductive organs, particularly the internal structures like the prostate and seminal vesicles are branches of the inferior vesical artery and the middle rectal artery. Both of these arteries are branches of the internal iliac artery.
Venous Drainage: Veins generally follow a similar path as the arteries, draining blood away from the reproductive organs. These veins eventually drain into the internal iliac vein.
Nervous Supply: The male reproductive system is innervated by both the sympathetic and parasympathetic nervous systems, which play important roles in regulating functions like ejaculation, erection, and glandular secretions.
Prostate Gland
The prostate is the largest accessory gland of the male reproductive system.
Location: Situated just below the bladder and surrounding the upper part of the urethra (the tube that carries urine and semen).
Structure: Composed of both glandular tissue (which produces prostatic fluid) and fibromuscular tissue (which provides structural support and helps with ejaculation).
Function:
Produces a significant portion of the seminal fluid, which mixes with sperm to form semen.
Prostatic fluid is slightly alkaline and helps to:
Neutralize the acidity of the male urethra and the female vagina, creating a more favorable environment for sperm survival.
Enhance sperm motility (movement).
Provide nutrients for sperm.
Bulbourethral Glands (Cowper’s Glands)
Structure: Two small, pea-sized glands.
Location: Situated below the prostate gland on either side of the urethra.
Function:
Secrete a clear, viscous fluid (pre-ejaculate) into the urethra during sexual arousal.
This fluid helps to:
Lubricate the urethra for the passage of semen.
Neutralize any residual acidity in the urethra from urine, further protecting sperm.
The Female Reproductive System
The Female External Genital Organs (Vulva)
The external female genitalia, collectively known as the vulva, include the following structures:
Mons Pubis
Labia Majora
Labia Minora
Vestibule
External Urethral Orifice
Vaginal Orifice
Greater Vestibular Glands (Bartholin’s Glands)
Lesser Vestibular Glands (Skene’s Glands)
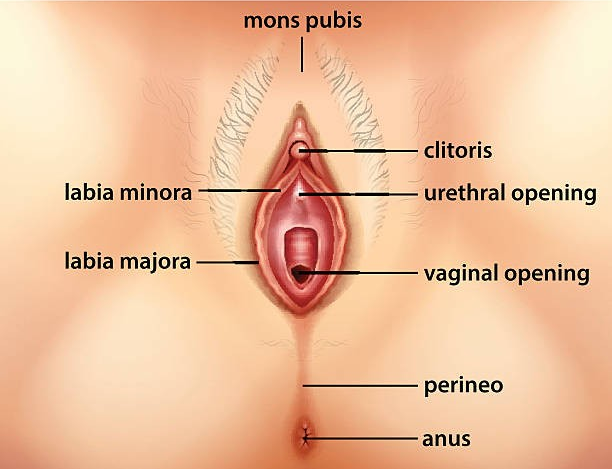
The Mons Pubis
A rounded elevation of fatty tissue located in front of the pubic symphysis.
Composed mainly of a pad of fatty connective tissue beneath the skin.
Fat content increases at puberty and decreases after menopause.
Covered with coarse pubic hair after puberty; hair thins after menopause.
Typically, the pubic hair distribution in females has a horizontal upper border.
The Labia Majora
Two symmetrical folds of skin that protect the urethral and vaginal openings.
Extend posteriorly from the mons pubis, filled with subcutaneous fat.
Located on either side of the pudendal cleft (the space between the labia majora).
Meet anteriorly at the anterior labial commissure.
Do not join posteriorly but are connected by a transverse bridge of skin called the posterior labial commissure.
The Labia Minora
Thin, delicate, hairless folds of skin located between the labia majora.
Contain a core of spongy tissue with many small blood vessels but no fat.
The internal surface has a pink, mucous membrane appearance.
Rich in sensory nerve endings.
Sebaceous and sweat glands open on both surfaces.
Enclose the vestibule of the vagina.
Meet superior to the clitoris, forming the prepuce (clitoral hood).
In young females, they may be joined posteriorly by a small fold of skin called the frenulum.
The Vestibule of the Vagina
The space between the labia minora.
Contains the openings of the urethra, vagina, and the ducts of the greater vestibular glands.
The External Urethral Orifice
A small opening located 2-3 cm behind the clitoris and just in front of the vaginal orifice.
The ducts of the paraurethral glands (Skene’s glands), which are comparable to the male prostate, are located on either side.
The Vaginal Orifice
A larger opening located below and behind the external urethral orifice.
Its size and appearance vary depending on the condition of the hymen, a thin fold of mucous membrane surrounding the opening.
The Greater Vestibular Glands (Bartholin’s Glands)
Approximately 0.5 cm in diameter.
Located on each side of the vestibule, posterolateral to the vaginal orifice.
Partly overlapped posteriorly by the bulbs of the vestibule.
Slender ducts from these glands open into the vestibule on each side of the vaginal orifice.
Secrete lubricating mucus during sexual arousal.
Comparable to the bulbourethral glands in the male.
The Clitoris
An erectile organ, 2-3 cm in length, comparable to the penis.
Not traversed by the urethra, therefore it lacks a corpus spongiosum.
Located behind the anterior labial commissure, usually hidden by the labia when flaccid.
Composed of a root and a body, including two crura, two corpora cavernosa, and a glans.
Suspended by a suspensory ligament.
The labia minora form the prepuce (hood) anterior to the clitoris and the frenulum posterior to it.
Enlarges upon tactile stimulation but does not lengthen significantly.
Highly sensitive and important for female sexual arousal.
Arterial Supply, Venous Drainage, and Lymph Drainage of the Female External Genitalia
Arterial Supply:
Rich blood supply from two external pudendal arteries and one internal pudendal artery on each side.
The internal pudendal artery supplies the skin, external genitalia, and perineal muscles.
Labial arteries, as well as the dorsal and deep arteries of the clitoris, are branches of the internal pudendal artery.
Venous Drainage:
Labial veins drain into the internal pudendal veins and accompany the internal pudendal artery.
Lymph Drainage:
The vulva has a rich network of lymphatic channels.
Most lymph vessels drain to the superficial inguinal lymph nodes and then to the deep inguinal nodes.
Diploma in Midwifery