Communicable Diseases
TETANUS
Table of Contents
Learning Objectives
- Describe the causative agent, epidemiology, and modes of transmission of tetanus.
- Explain the mechanism of action of tetanospasmin and its effect on the central nervous system.
- Recognize the clinical features, characteristic signs, and different types of tetanus, including generalized, local, and neonatal.
- Outline the clinical approach to diagnosing tetanus and list key differential diagnoses.
- Summarize the main principles of tetanus treatment, including toxin neutralization, spasm control, and supportive care.
- Detail the strategies for tetanus prevention through active and passive immunization, including post-exposure prophylaxis.
TETANUS
INTRODUCTION
- Tetanos – a greek word – to strech
- First described by Hippocrates & Susruta
- Tetanus an neurological disease characterized by an acute onset of hypertonia, painful muscular contractions (usually of the muscles of the jaw and neck), and generalized muscle spasms without other apparent medical causes.
- Only vaccine preventable disease that is infectious but not contagious
CAUSATIVE AGENT
- Caused by CLOSTRIDIUM TETANI
- Anaerobic
- Motile
- Gram positive bacilli
- Oval, colourless, terminal spores – tennis racket or drumstick shape.
- It is found worldwide in soil, in inanimate environment, in animal faeces & occasionally human faeces.
Clostridium tetani Gram Stain
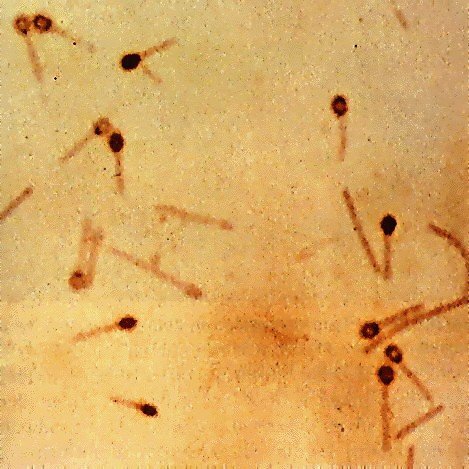
NOTE: Round terminal spores give cells a “drumstick” or “tennis racket” appearance.
EPIDEMIOLOGY
- Tetanus is an international health problem, as spores are ubiquitous. The disease occurs almost exclusively in persons who are unvaccinated or inadequately immunized.
- Entirely preventable disease by immunization
- Tetanus occurs worldwide but is more common in hot, damp climates with soil rich in organic matter.
- More common in developing and under developing countries.
- More prevalent in industrial establishment, where agricultural workers are employed.
- Tetanus neonatorum is common due to lack of MCH Care
India
Tetanus is important endemic infection in India.
Causative factors
- Hand washing
- Delivery practices
- Traditional birth customs
- Interest in immunization
Prior to the national immunization programme estimated 3.5 lakh children were dying annually. 70,000 cases continue to occur largely in the states – Orissa, Bihar, MP, Aasam, Rajasthan, UP ,where TT immunization coverage is less than national coverage(70%).
TRANSMISSION
Tetanus is not transmitted from person to person. Infection occurs when C. tetani spores are introduced into acute wounds from trauma, surgeries and injections, or chronic skin lesions and infections. Cases have resulted from wounds that were considered too trivial to warrant medical attention. The incubation period of tetanus is usually between three and 21 days (median 7 days). Shorter incubation periods (<7 days) along with delays in seeking treatment are associated with fatal outcomes. Outbreaks of tetanus related to injuries associated with natural disasters such as earthquakes and tsunamis have been documented²˒³.

Host Factors
- Age : It is the disease of active age (5-40 years), New born baby, female during delivery or abortion
- Sex : Higher incidence in males than females
- Occupation : Agricultural workers are at higher risk
- Rural –Urban difference: Incidence of tetanus in urban areas is much lower than in rural areas
- Immunity : Herd immunity does not protect the individual
- Environmental and social factors: Unhygienic custom habits,Unhygienic delivery practices
ROUTE OF ENTRY
- Apparently trivial injuries
- Animal bites/human bites
- Open fractures
- Burns
- Gangrene
- In neonates usually via infected umbilical stumps
- Abscess
- Parenteral drug abuse

TETANUS PRONE WOUND
- A wound sustained more than 6 hr before surgical treatment.
- A wound sustained at any interval after injury which is puncture type or shows much devitalised tissue or is septic or is contaminated with soil or manure.
Sporulated
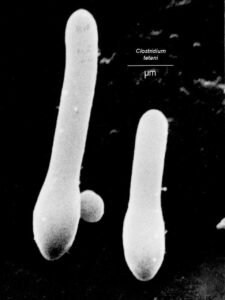
Vegetative
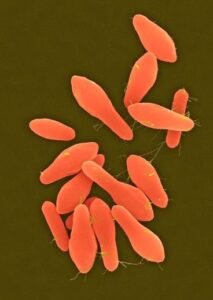
- Spores that gain entry can persist in normal tissue for months to years under anaerobic conditions.
- When the oxygen levels in the surrounding tissue is sufficiently low, the implanted C. tetani spore then germinates into a new, active vegetative cell that grows and multiplies and most importantly produces tetanus toxin – tetanospasmin and tetanolysin.*
- Tetanolysin is not believed to be of any significance in the clinical course of tetanus.
- Tetanospasmin is a neurotoxin and causes the clinical manifestations of tetanus.
- The toxin migrates across the synapse (small space between nerve cells critical for transmission of signals among nerve cells) where it binds to presynaptic nerve terminals and inhibits or stops the release of certain inhibitory neurotransmitters (glycine and gamma-amino butyric acid).
- Loss of inhibition of preganglionic sym neurons – sympathetic hyperactivity
- These neurons become incapable to release neurotransmitter. The neurons, which release gamma-aminobutyric acid (GABA) and glycine, the major inhibitory neurotransmitters, are particularly sensitive to tetanospasmin, leading to failure of inhibition of motor reflex responses to sensory stimulation.
- This results in generalized contractions of the agonist and antagonist musculature characteristic of a tetanic spasm.
- The shortest peripheral nerves are the first to deliver the toxin to the CNS, which leads to the early symptoms of facial distortion and back and neck stiffness.
- Once the toxin becomes fixed to neurons, it cannot be neutralized with antitoxin. Recovery of nerve function from tetanus toxins requires sprouting of new nerve terminals and formation of new synapses.
Mechanism of Action of Tetanus Toxin
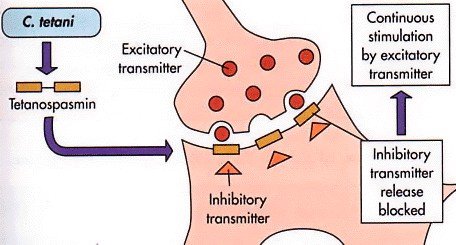
- C. tetani enters body from through wound.
- Stays in sporulated form until anaerobic conditions are presented.
- Germinates under anaerobic conditions and begins to multiply and produce tetnospasmin.
- Tetnospasmin spreads using blood and lymphatic system, and binds to motor neurons.
- Travels along the axons to the spinal cord.
- Binds to sites responsible for inhibiting skeletal muscle contraction.
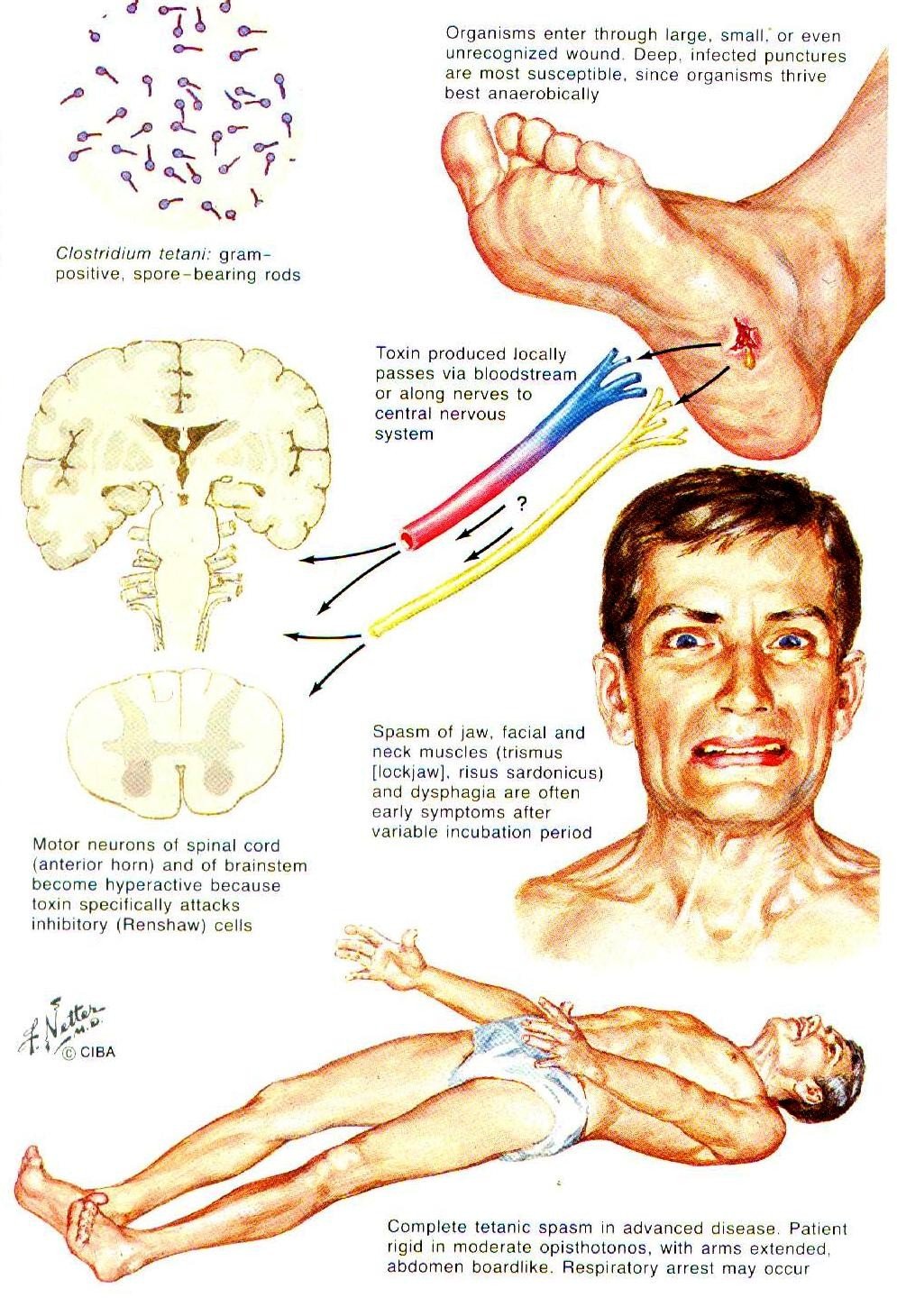
- Spores are extremely stable,although immersion in boiling water for 15 minutes kills most spores. Exposure to saturated steam under 15 lbs.of pressure for 15-20 minutes at 121°c is highly effective against spores.
- Sterilization by dry heat is slower than by moist heat (1 -3 hrs at 160 °C),but it is also effective against spores.
- Ethylene oxide sterilization is also sporocidal.
- Autoclaving at 121°C for 15min kills the spores readily.
- Iodine(1% aqueous soon) and H2O2 (10 volume)
CLINICAL FEATURES:
- IP : Time from injury to the first symptom.The median incubation period is 7 days, and, for most cases (73%), incubation ranges from 3-21 days.
- Period of onset : It is the time from first symptoms to the reflex spasm.
- In general the further the injury site is from the central nervous system, the longer the incubation period.
- The shorter the incubation period, the higher the chance of death.
- Triad of muscle rigidity, spasms & autonomic dysfunction
- Early symptoms are neck stiffness, sore throat and poor mouth opening.
- Patients with generalized tetanus present with trismus (ie, lockjaw) in 75% of cases.
- Other presenting complaints include stiffness, neck rigidity, dysphagia, restlessness, and reflex spasms. Spasms usually continue for 3-4 weeks.
- Subsequently, muscle rigidity becomes the major manifestation. Rigid Abdomen.
- Muscle rigidity spreads in a descending pattern from the jaw and facial muscles over the next 24-48 hours to the extensor muscles of the limbs – stiff proximal limb muscles & relatively
TRISMUS
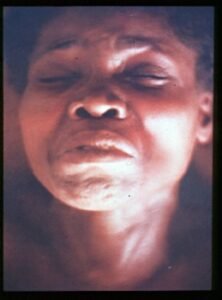
- Risus sardonicus: Sustained contraction of facial musculature produces a sneering grin expression known as risus sardonicus.
- Contraction of the muscles at the angle of mouth and frontalis
- Trismus (Lock Jaw): Spasm of Masseter muscles.
- Opisthotonus: Spasm of extensor of the neck, back and legs to form a backward curvature.
- Muscle spasticity
- Poor cough, inability to swallow, gastric stasis all increase the risk of aspiration. Respiratory failure continues to be a major cause of mortality in developing countries, whereas severe autonomic dysfunction causes most deaths in the developed world.
RISUS SARDONICUS
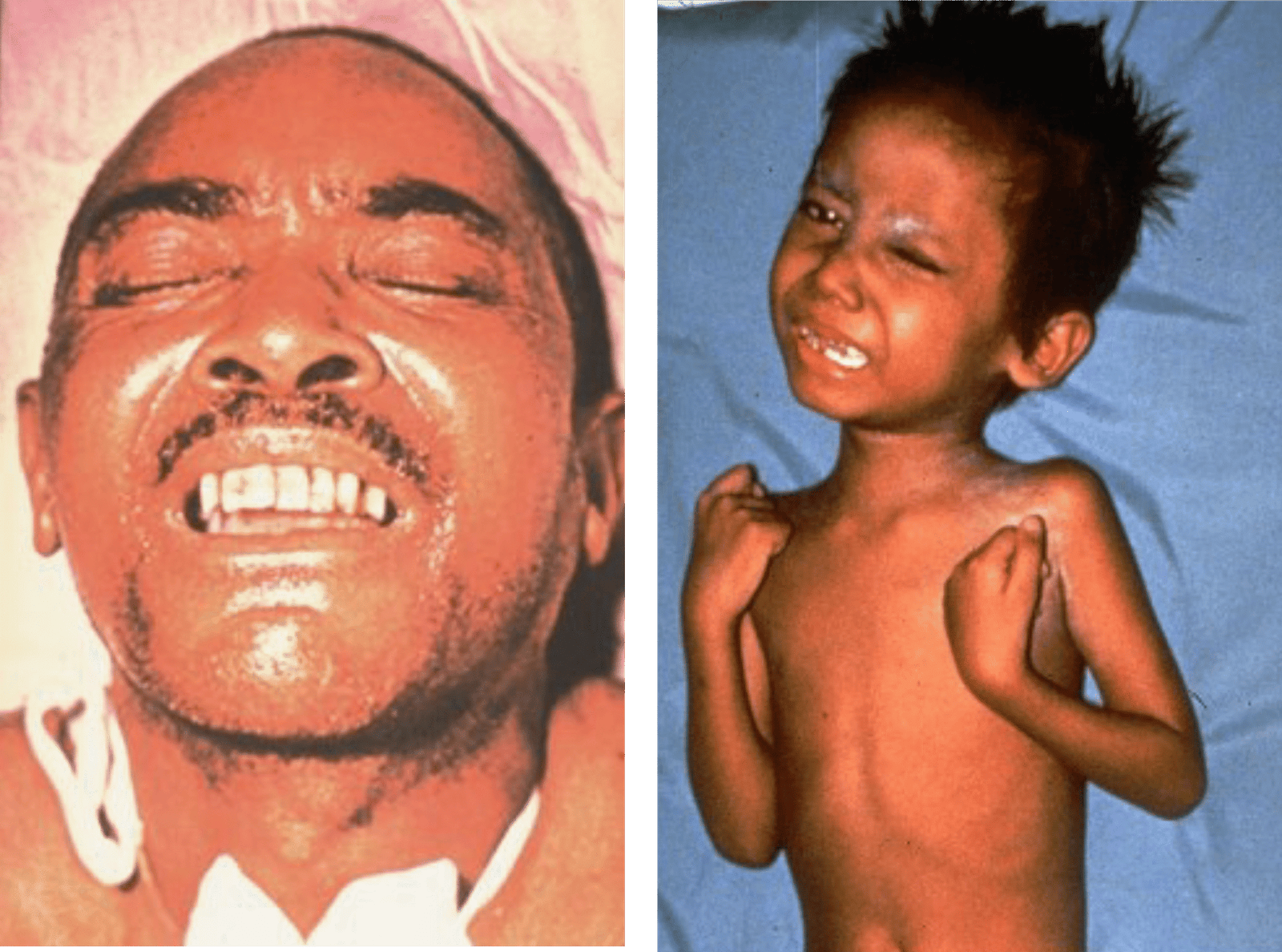
Opisthotonos in Tetanus Patient

The contractions by the muscles of the back and extremities may become so violent and strong that bone fractures may occur

- Dysphagia occurs in moderately severe tetanus due to pharyngeal muscle spasms, and onset is usually insidious over several days.
- Reflex spasms develop in most patients and can be triggered by minimal external stimuli such as noise, light, or touch. The spasms last seconds to minutes; become more intense; increase in frequency with disease progression; and can cause apnea, fractures, dislocations, and rhabdomyolysis.
- Laryngeal spasms can occur at any time and can result in asphyxia.
AUTONOMIC DYSFUNCTION
- Tetanospasmin has a disinhibitory effect on the autonomic nervous system (ANS) due to increased release of catecholamines it causes :
- Hyperpyrexia
- Sweating
- Peripheral vasoconstriction
- Labile/Sustained Hypertension
- Episodic tachycardia, dysrhythmias and cardiac arrest
- Occasionally period of bradycardia & hypotension
Other symptoms include:
- Drooling
- Fever usually absent
- Mentation unimpaired
- Hand or foot spasms
- Irritability
- Uncontrolled urination or defecation
Duration of illness — Tetanus toxin-induced effects are long-lasting because recovery requires the growth of new axonal nerve terminals. The usual duration of clinical tetanus is four to six weeks.
SEQUENCE OF EVENTS
Lock Jaw Stiff Neck Difficulty Swallowing Muscle Rigidity Spasms
TYPES OF TETANUS
- Generalied vs Local
- Cephalic
- Traumatic
- Otogenic
- Idiopathic
- Puerperal
- Tetanus neonatorum
Maternal tetanus
- Tetanus occurring during pregnancy or within 6 weeks after any type of pregnancy termination, is one of the most easily preventable causes of maternal mortality.
- It includes postpartum or puerperal tetanus
- (i) postpartum or puerperal tetanus, usually resulting from septic procedures during delivery,
- (ii) postabortal tetanus, following septic maneuvers during induced abortion
- (iii) Tetanus during pregnancy, generally resulting from inoculation through a nongenital portal of entry
NEONATAL TETANUS
- Tetanus neonatorum (8th day disease)
- Usually fatal if untreated
- Children born to inadequately immunized mothers, after unsterile treatment of umbilical stump
- During first 2 weeks of life.
- Poor feeding ,rigidity and spasms
- It is easily preventable by 2 tetanus toxoid injections and ‘5 cleans’ while conducting deliveries.

LOCAL TETANUS
- Uncommon form
- Manifestations are restricted to muscles near the wound.
- Cramping and twisting in skeletal muscles surrounding the wound – local rigidity
- Prognosis – excellent
CEPHALIC TETANUS
- A rare form of local tetanus
- Follows head injury / ear infection
- Involves one / more facial cranial nerves
- Trismus and localised paralysis ,usually facial nerve, often unilateral.
- Involvement of cranial nerves VI,III, IV, and XII may also occur either alone or in combination with others
- Incubation period : few days
- Mortality : high
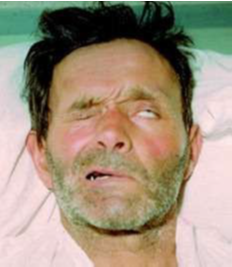
Ophthalmoplegic tetanus is a variant that develops after penetrating eye injuries and results in CN III palsies and ptosis.
DIAGNOSIS
- There are currently no blood tests that can be used to diagnose tetanus. Diagnosis is done clinically based on the presence of trismus, dysphagia, generalized muscular rigidity, and/or spasm.
- Laboratory studies may demonstrate a moderate peripheral leukocytosis.
- An assay for antitoxin levels is not readily available. However, a level of 0.01 IU/mL or greater in serum is generally considered protective, making the diagnosis of tetanus less likely.
- Cerebrospinal fluid (CSF) study findings are usually within normal limits.
DIRECT SMEAR
- Show Gram-positive bacilli with drum-stick appearance.
- Morphologically indistinguishable from similar nonpathogenic bacilli.
CULTURE
- Done in blood agar under anaerobic condition or in Robertson’s cooked meat medium.
- Produces swarming growth after 1-2 days of incubation.
- In contaminated specimen heat at 80°C for 10mins before culture to destroy non-sporing organisms.
ANIMAL INOCULATION
- To demonstrate toxigenicity.
- Positive case : test animal develops stiffness & spasm of tail & inoculated hind limb within 12-24hrs which spreads to rest of the body. Death occurs in 1-2 days.
Procedures:
- The spatula test is one diagnostic bedside test.
- This simple test involves touching the oropharynx with a spatula or tongue blade.
- This test typically elicits a gag reflex, and the patient tries to expel the spatula (ie, a negative test result).
- If tetanus is present, patients develop a reflex spasm of the masseters and bite the spatula (ie, a positive test result).
- Sensitivity of 94% and a specificity of 100%.
- No adverse sequelae (eg, laryngeal spasm) from this procedure were reported
DIFFERENTIAL DIAGNOSIS
- Drug induced Dystonic Reactions e.g. Phenothiazines
- Strychnine poisoning
- Neuroleptic Malignant Syndrome, Serotonin syndrome
- Trismus d/t Peritonsillar Abscess/Dental infection
- Stiff person syndrome
- Acute abdominal emergencies
- Dislocations, Mandible
- Encephalitis, Meningitis
- Hysteria
- Hypocalcemia
- Rabies
- Seizure disorder (partial or generalized)
- Spider Envenomations, Widow
- Stroke, Hemorrhagic
- Stroke, ischemic (cephalic tetanus)
PRINCIPLE OF TREATMENT
- Neutralization of unbound toxin -HTIG/ATS
- Prevention of further toxin production -Wound debridement & antibiotics
- Antibiotics
- Control of spasm -Anticonvulsants, Sedatives, Muscle relaxants etc.
- Management of autonomic dysfunction -MGSO4, Betablockers etc.
- Supportive care -Physiotherapy, Nutrition, Thromboembolism prophylaxis ABC etc…
PRINCIPLE OF TREATMENT
- Admit patients to the intensive care unit (ICU).
- Because of the risk of reflex spasms, maintain a dark and quiet environment for the patient. Avoid unnecessary procedures and manipulations.
- Attempting endotracheal intubation may induce severe reflex laryngospasm; prepare for emergency tracheostomy.
- Seriously consider prophylactic tracheostomy in all patients with moderate-to-severe clinical manifestations. Intubation and ventilation are required in 67% of patients.
- Tracheostomy has also been recommended after onset of the first generalized seizure.
TOXIN
- A single intramuscular dose of 3000-5000 units (100U/kg-half in each buttocks) is generally recommended for children and adults, with part of the dose infiltrated around the wound if it can be identified.
- The WHO recommends TIG 500 units by IM/IV (depending on the available preparation) as soon as possible; in addition, administer age-appropriate TT-containing vaccine (Td, Tdap, DT, DPT, DTaP, or TT depending on age or allergies), 0.5 cc by intramuscular injection at separate site with HTIG.
- TIG can only help remove unbound tetanus toxin, but it cannot affect toxin bound to nerve endings.
- 250 U/vial available in our hospital, so 10 vial in
PREVENTION OF FURTHER TOXIN PRODUCTION
- Debridement of Wound to remove organisms and to create an aerobic environment.
- The current recommendation is to excise at least 2 cm of normal viable-appearing tissue around the wound margins.
- Incise and drain abscesses.
- Delay any wound manipulation until several hours after administration of antitoxin due to risk of releasing tetanospasmin into the bloodstream.
ANTIBIOTICS
- Theoretically, antibiotics may prevent multiplication of C tetani, thus halting production of toxin. Penicillin G was the drug of choice initially but now Metronidazole is preffered drug.
- Penicillin G aqueous : (10-12 MU IV in 2-4 divided doses- 2-4 MU IV every 4 to 6 hrs)
- A 10- to 14-d course of treatment is recommended
- Metronidazole: (5oomg 6 hrly or 1gm 12 hrly)
- A 10- to 14-d course of treatment is recommended. Some consider this the DOC since penicillin G is also a GABA agonist, which may enhance effects of the toxin.
- Doxycycline, Clindamycin and Erythromycin are alternative for penicillin allergic patients who can not
Control of spasm
- Nursing in quiet environment, avoid unnecessary stimuli, Protecting the airway.
- Drugs used to treat muscle spasm, rigidity, and tetanic seizures include sedative-hypnotic agents, general anesthetics, centrally acting muscle relaxants, and neuromuscular blocking agents.
- Anticonvulsants
- Sedative-hypnotic agents are the mainstays of tetanus treatment. Benzodiazepines are the most effective primary agents for muscle spasm prevention and work by enhancing GABA inhibition.
Diazepam :
- Mainstay of treatment of tetanic spasms and tetanic seizures. Depresses all levels of CNS, including limbic and reticular formation, possibly by increasing activity of GABA, a major inhibitory neurotransmitter.
- Diazepam reduces anxiety, produces sedation, and relaxes muscles. Lorazepam is an effective alternative. Large amounts of either may be required (up to 600 mg/d).
- Diazepam or Midazolam can be used as 5-10mg iv/im every 1-4 hrly.
- Midazolam can be given as an intravenous infusion (5 -15 mg/hr).
- Phenobarbitone (up to 200 mg IV or PO/NG 12-hourly), and phenothiazines (usually chlorpromazine-25mg/ml, 100mg IM f/b 50-100mg 12hrly) may be added as an adjunctive sedative.
- Propofol, dantrolene, intrathecal baclofen, succinylcholine & magnesium sulfate can be tried
Skeletal muscle relaxants:
- These agents can inhibit both monosynaptic and polysynaptic reflexes at spinal level, possibly by hyperpolarization of afferent terminals.
- Muscle relaxation is indicated where sedation alone is inadequate. Vecuronium (0.1 mg/kg IV as needed) or atracurium (0.5 mg/kg IV) are appropriate.
- Pancuronium may worsen autonomic instability by inhibiting catecholamine reuptake.
- Prolonged usage of aminosteroid muscle relaxants has been associated with critical illness neuropathy and myopathy.
BACLOFEN
- Intrathecal (IT) baclofen, a centrally acting muscle relaxant, has been used experimentally to wean patients off the ventilator and to stop diazepam infusion. IT baclofen is more potent than PO baclofen.
- May induce hyperpolarization of afferent terminals and inhibit both monosynaptic and polysynaptic reflexes at spinal level.
- Entire dose of baclofen is administered as a bolus injection. Dose may be repeated after 12 h or more if spontaneous paroxysms return.
- It can also be given as T. Baclofen 5mg tds, increase 5mg/day every 3 days,maximum dose 80mg
DRIP RATE OF COMMON DRUGS
- Diazepam 1 Amp. = 2 ml = 10 mg ( 5 mg / ml )
- 5Amp in 50cc (40+10) NS – 50mg/50ml = 1mg/ml
- Usually needed 5-10ml/hr (10ml/hr=240mg/hr), may need even more than that.
- Ideally not given by continuous infusion because of precipitation in IV fluids & absorption of drug into infusion bags & tubing. Usually 10-40mg every 1-8 hours needed.
- Midazolam 1 vial = 5 ml = 5 mg ( 1 mg / ml)
- 10 vial = 50cc @ 5ml/hr (=5mg/hr)
- Usually 5-15mg/hr (5-15ml/hr) needed
Atracurium 1 Amp. = 2.5 ml = 25 mg ( 10 mg / ml)
- 8Amp in 500cc NS/5%DW = 0.4mg/ml = 200mg
- 1 Amp (0.5mg/kg=25mg) IV stat f/b 5-10 µg/kg/min= 0.25-0.5 mg/min = 15-30 mg/hr = 37.5-75ml/hr
- Maintainance dose : 11-13 µg/kg/min
- For infusion pump in 50cc, divide drip rate by 10.
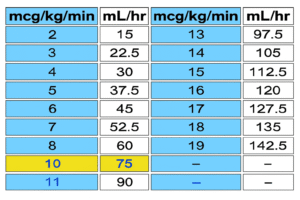
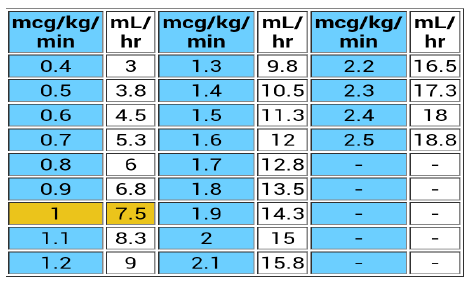
Vecuronium 1 Vial = 4 mg to be reconstituted with 2 ml of sterile water = (2 mg / ml)
- 5 vial in 50 cc NS/5%DW = 20mg = 0.4mg/ml
- 0.1mg/kg bolus = 5mg = 2.5 ml f/b 0.8 -1.7 µg/kg/min (1 µg/kg/min = 50µg/min = 3mg/hr = 7.5 ml/hr
- Maintainance dose : 0.8 – 1.2 µg/kg/min
METHOCARBAMOL (ROBINAX)
- May be used as adjunct but not much useful in tetanus.
- Skeletal muscle relaxant
- 100mg/ml , 10ml/vial – total 1gm/vial
- Tablet : 500/750mg
- IV : 1-2gm direct IV injection (at 3ml/min = 300mg/min). Additional 1-2gm IV infusion for total dose of 3gm initially.May repeat 1-2 gm IV every 6 hourly untill can give TRT/PO. Injection should not be used for more than 3 consecutive days. Total oral daily dose upto 24gm may be neded.
- Oral : 1.5-2.0 gm QID for 48-72 hrs, then
MANAGEMENT OF AUTONOMIC DYSFUNCTION:
Fluid loading is a useful in minimizing autonomic instability.
Magnesium Sulphte:
- It is an effective adjunct in relaxation , sedation & controlling the autonomic disturbance in tetanus.
- It is a pre-syneptic neuromuscular blocker, reduces catecholemine release from nerves & adrenal medulla; and reduces responciveness to released catechlemines.
- A loading dose of 5gm should be given over 20 minutes, followed by intravenous infusion of 2gm/hr. the dose can be incresed by upto 0.5g/hr until spasms are relieved or the patellar reflex disappears.
- If infusion devices are unavailable , give 2.5gm i.v. every 2 hours , titrating the frequency of administration to spasms.
- To avoid overdose, monitor patellar reflex as areflexia(absence of patellar reflex) occurs at the upper end of the therapeutic range (4mmol/L). If areflexia develops, dose should be decreased.
- By antagonizing the calcium metabolism MgSO4 causes weakness & paralysis in overdose. Monitoring of serum magnesium level is important to prevent this: the normal serum magnesium level is 0.7- 1.0 mmol/l & acceptable therapeutic level is 2-3.5 mmol/l.
Another drugs:
- Labetalol
- Continuous infusion of esmolol
- Clonidine / verapamil
SUPPORTIVE CARE
► Airway management and other supportive measures —
Since tetanus toxin cannot be displaced from the neuromuscular junction once bound, supportive care is the main treatment for tetanus. In patients with severe tetanus, prolonged immobility in the intensive care unit is common, much of which is in mechanical ventilation and may last for weeks. Such patients are predisposed to nosocomial infections, decubitus ulcers, tracheal stenosis, gastrointestinal hemorrhage, and thromboembolic disease.
► Endotracheal intubation is justified initially, but early tracheostomy is recommended because of the likelihood of prolonged mechanical ventilation. The latter allows better tracheal suctioning and pulmonary toilet.
► Energy demands in tetanus may be extremely high, so early nutritional support is mandatory. Enteral feeding is preferred if enough calories can be administered by this route. Placement of PEG tubes is sometimes needed, since this route may prevent gastroesophageal reflux, which may be induced by nasogastric tubes. Prophylactic treatment with sucralfate or acid blockers may be used to prevent gastroesophageal hemorrhage from stress ulceration.
►For patients needing artificial ventilation, steps should be taken to prevent ventilator-associated pneumonia, such as nursing in the semi-recumbent position. Prevention of respiratory complications by chest physiotherapy, mouth care and regular tracheal suctioning may be necessary due to increased secretions.
►Prophylaxis of thromboembolism with heparin, low molecular weight heparin or other anticoagulants should be administered early.►Physical therapy should be started as soon as spasms have ceased, since tetanus patients often are left with disability from prolonged drug-induced paralysis and immobilization.
PREVENTION
- Tetanus is completely preventable by active tetanus immunization.
- Immunization is thought to provide protection for 10 years.
- Begins in infancy with the DTP series of shots. The DTP vaccine is a “3-in-1” vaccine that protects against diphtheria, pertussis, and tetanus.
IMMUNIZATION
- 1st dose – 6th week (DPT)
- 2nd dose – 10th week (DPT)
- 3rd dose – 14th week (DPT)
- 1st booster – 18th month (DPT)
- 2nd booster – 6th year (DT)
- 3rd booster – 10th year (TT)
MONOVALENT VACCINES
- Purified tetanus toxoid ( adsorbed ) supplanted the plain toxoid – higher & long lasting immunity response
- Primary course of immunization – 3 doses
- Each 0.5 ml , injected into arm given at intervals of 0,1,6 months
- The longer the interval b/w two doses, better is the immune response
- Booster doses : After 1 yr f/b Every 10 yrs
- Older teenagers and adults who have sustained injuries, especially puncture-type wounds, should receive booster immunization for tetanus if more than 10 years have passed since the last booster.
- Recovered clinical tetanus does not produce immunity to further attacks because very small amount of tetanus toxin produced can not elicit strong protective immune response.Therefore, even after recovery patients must receive a full course of tetanus toxoid.
POSTEXPOSURE PROPHYLAXIS:
All wound receive surgical toilet
A – has had a complete course of toxoid or booster dose with in the past 5 year B – has had a complete course of toxoid or booster dose more then 5 years ago & less then 10 years ago C – has had a complete course of toxoid or a booster dose more then 10 year ago D – has not had a complete course of toxoid or immunity status unknown
PASSIVE IMMUNIZATION
- Temp protection – human tetanus immunoglobulin /ATS
Human Tetanus Hyperimmunoglobulin :
- 250-500 IU
- Produces protective antibody level for atleast 4-6 weeks.
- Does not cause serum sickness
- Longer passive protection compared to horse ATS( 30 days / 7 -10 days )
PASSIVE IMMUNIZATION
ATS ( EQUINE ):
- 1500 IU s/c after sensitivity testing
- 7 – 10 days
- High risk of serum sickness
- It stimulates formation of antibodies to it , hence a person who has once received ATS tends to rapidly eliminate subsequent doses.
ACTIVE & PASSIVE IMMUNIZATION
- In non immunized persons
- 1500 IU of ATS / 250-500 units of Human Ig in one arm & 0.5 ml of adsorbed tetanus toxoid into other arm /gluteal region
- 6 wks later, 0.5 ml of tetanus toxoid
- 1 yr later , 0.5 ml of tetanus toxoid
PREVENTION OF NEONATAL TETANUS
- Clean delivery practices
- 3 cleans : clean hands, clean delivery surface, clean cord care
- Tetanus toxoid protects both mother & child
- Unimmunized pregnant women : 2 doses tetanus toxoid (16th-36th week)
- 1st dose as early as possible during pregnancy
- 2nd dose – at least a month later / 3 wks before delivery
- Immunized pregnant women : a booster is sufficient
- No need of booster in every consecutive pregnancy
- To newborn of unimmunized mother, 500U HTIG
Join Our WhatsApp Groups!
Are you a nursing or midwifery student looking for a space to connect, ask questions, share notes, and learn from peers?
Join our WhatsApp discussion groups today!
Join NowWe are a supportive platform dedicated to empowering student nurses and midwives through quality educational resources, career guidance, and a vibrant community. Join us to connect, learn, and grow in your healthcare journey
Quick Links
Our Courses
Legal / Policies
Get in Touch
(+256) 790 036 252
(+256) 748 324 644
Info@nursesonlinediscussion.com
Kampala ,Uganda
© 2026 Nurses online discussion. All Rights Reserved




