Gnaecology and Reproductive health
Structural Abnormalities of the Female Genital Tract
Table of Contents
Definition
Structural abnormalities of the female genital tract refer to congenital or acquired deviations from the normal anatomy of the reproductive organs. These abnormalities may affect the vulva, vagina, cervix, uterus, fallopian tubes, or ovaries, and can lead to menstrual irregularities, infertility, pain, or obstetric complications.
I. Congenital Abnormalities
These arise due to improper development, fusion, or resorption of the Müllerian ducts during embryogenesis.
A. Vaginal Abnormalities
Imperforate Hymen: Failure of hymen perforation; leads to hematocolpos.
Transverse Vaginal Septum: Horizontal tissue obstructs vaginal canal.
Vaginal Agenesis: Absence of vaginal canal, often associated with uterine agenesis.
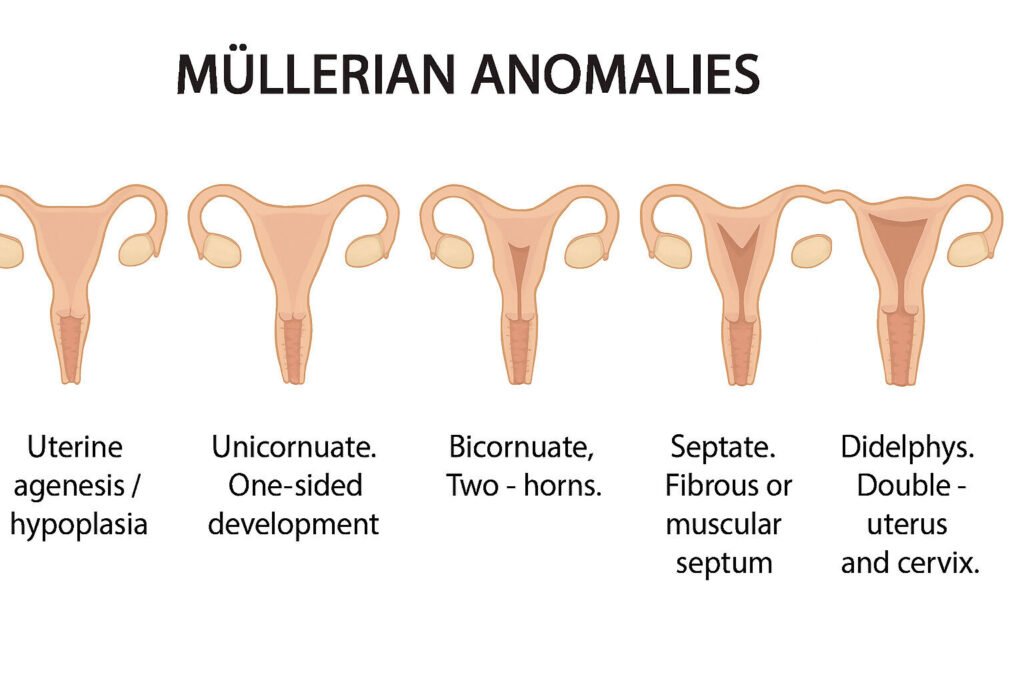
B. Uterine Abnormalities
Uterine Agenesis/Hypoplasia: Complete or partial absence of uterus.
Unicornuate Uterus: One-sided development due to incomplete duct formation.
Bicornuate Uterus: Two horns due to partial fusion failure.
Septate Uterus: Fibrous or muscular septum divides uterine cavity.
Didelphys Uterus: Complete failure of fusion; two uteri and cervices.
C. Cervical and Tubal Abnormalities
Cervical Atresia: Absence or blockage of cervical canal.
Tubal Agenesis or Duplication: Absence or duplication of fallopian tubes.
II. Acquired Structural Abnormalities
These develop due to trauma, infection, surgery, or disease.
A. Uterine Fibroids (Leiomyomas)
Benign tumors of uterine muscle.
Can distort uterine shape and impair fertility.
B. Endometriosis
Ectopic endometrial tissue growth.
Causes adhesions and anatomical distortion.
C. Pelvic Organ Prolapse
Descent of uterus, bladder, or rectum due to weakened pelvic floor.
D. Fistulas
Abnormal connections between genital tract and adjacent organs.
Vesico-vaginal fistula: Between bladder and vagina.
Recto-vaginal fistula: Between rectum and vagina.
E. Post-Surgical or Traumatic Scarring
From procedures like dilation and curettage (D&C), cesarean section, or perineal tears.
III. Clinical Features
Primary amenorrhea (in congenital absence or obstruction).
Dysmenorrhea or cyclical abdominal pain.
Infertility or recurrent miscarriage.
Dyspareunia (painful intercourse).
Urinary or fecal incontinence (in fistulas).
Pelvic pain or pressure (in fibroids or endometriosis).
IV. Diagnosis
History and physical examination.
Pelvic ultrasound: First-line imaging.
MRI: Detailed soft tissue evaluation.
Hysterosalpingography (HSG): Uterine and tubal assessment.
Laparoscopy/Hysteroscopy: Direct visualization and treatment.
V. Management
Surgical correction:
Septum resection
Metroplasty
Fistula repair
Hormonal therapy:
For endometriosis or menstrual regulation
Assisted reproductive techniques:
IVF for severe anomalies
Supportive care:
Counseling
Pelvic floor therapy
Join Our WhatsApp Groups!
Are you a nursing or midwifery student looking for a space to connect, ask questions, share notes, and learn from peers?
Join our WhatsApp discussion groups today!
Join NowWe are a supportive platform dedicated to empowering student nurses and midwives through quality educational resources, career guidance, and a vibrant community. Join us to connect, learn, and grow in your healthcare journey
Quick Links
Our Courses
Legal / Policies
Get in Touch
(+256) 790 036 252
(+256) 748 324 644
Info@nursesonlinediscussion.com
Kampala ,Uganda
© 2026 Nurses online discussion. All Rights Reserved

