Introduction to Midwifery
Ophthalmia neonatorum
Table of Contents
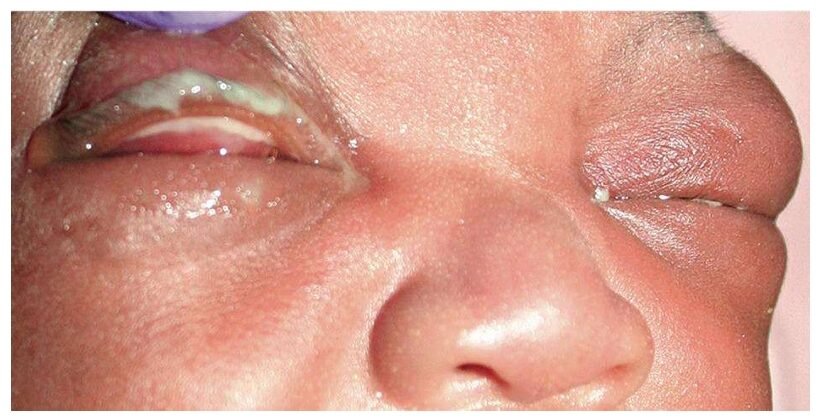
Definition
Ophthalmia neonatorum (ON) is a purulent (pus-containing) conjunctivitis occurring in the first month of life. It’s an inflammation of the conjunctiva (the membrane lining the inside of the eyelids and covering the sclera – the white part of the eye).
Causes Workflow
Bacterial Causes
- Neisseria gonorrhoeae (gonococcal ophthalmia neonatorum)
- Chlamydia trachomatis (chlamydial ophthalmia neonatorum)
- Staphylococcus aureus
- Streptococcus pneumoniae
- Haemophilus influenzae
- Others Gonococcal and chlamydial infections are the most serious and potentially blinding.
Viral Causes
- Herpes simplex virus (HSV)
- Adenoviruses
- Others These are less common causes but can also lead to severe complications.
Chemical Causes
- Soap
- Medications
- Other substances accidentally introduced into the eyes This is less severe than infectious causes.
Presentation Workflow
Common Features
- Eyelid swelling: Often the first sign, varying in severity from mild edema to significant swelling that may make it difficult to open the eyes.
- Discharge: Purulent (thick, yellow-green) discharge is characteristic of bacterial infections, while chlamydial infections may present with a less purulent, watery discharge that can become purulent later.
- Conjunctival redness (hyperemia): The conjunctiva will appear inflamed and red.
- Photophobia (light sensitivity): The infant may cry when exposed to light.
- Corneal involvement: In severe cases, the cornea (the transparent front part of the eye) can become cloudy or ulcerated, leading to permanent vision impairment or blindness. This is particularly true with gonococcal infections.
Prevention Workflow
Antenatal Prevention
- Regular screening for vaginal infections: Conduct regular examinations to detect vaginal discharges indicative of infections like gonorrhea and chlamydia.
- Treatment of vaginal infections: Ensure prompt and appropriate treatment of any identified vaginal infections in pregnant women using appropriate antibiotics.
- Management of high-risk pregnancies: Address conditions that may increase the risk of premature labor or prolonged rupture of membranes.
- Prevention and management of anemia: Address maternal anemia, as it can weaken the immune system and increase the risk of infection.
- Health education: Educate mothers on the importance of hygiene, including handwashing, perineal cleanliness, and avoidance of touching the eyes unnecessarily.
Intrapartum Prevention
- Sterile technique: Maintain strict sterile techniques during labor and delivery. All personnel should practice thorough hand hygiene.
- Avoid unnecessary eye swabbing: Avoid routine swabbing of the baby’s eyes during delivery unless absolutely necessary, as this can introduce infection. If swabbing is deemed necessary (e.g., for assessment), use separate sterile swabs for each eye, cleaning from the inner canthus outward.
- Isolation of infected mothers: Isolate mothers with purulent vaginal discharge to prevent transmission.
- Prophylactic antibiotics for prolonged rupture of membranes: Consider prophylactic antibiotics for mothers with prolonged rupture of membranes (PROM) exceeding 12 hours to reduce the risk of neonatal infection.
Postnatal Prevention
- Hand hygiene: Healthcare providers should perform thorough handwashing before and after handling newborns.
- Eye cleaning: Cleanse the baby’s eyes with sterile water or half-strength saline solution using a separate sterile cotton swab for each eye, cleaning from the inner to the outer canthus. Discard swabs after use.
- Avoid contact with birth fluids: Prevent the baby’s face from coming into contact with amniotic fluid.
- Educate mothers: Instruct mothers on proper hand hygiene before handling the baby and avoid touching the baby’s eyes.
- Prophylactic eye drops (during epidemics): In areas experiencing outbreaks of ophthalmia neonatorum, consider prophylactic eye drops (e.g., 1% silver nitrate or 10% sulfacetamide) immediately after birth. This practice is debated and requires careful consideration of potential side effects and local guidelines.
Management Workflow
Aims of Management
- Eradicate the infection.
- Prevent corneal damage and scarring.
- Preserve vision.
- Prevent transmission to others (e.g., other family members).
Management in Maternity Centre (Limited to Mild Cases ONLY – Referral is usually necessary)
- Admission and Isolation: Admit the baby and isolate them to prevent infection spread. Position the baby on its side with the affected eye downward. Use mosquito nets to protect the baby from flies. Separate and disinfect all used materials before sending them to the laundry.
- Eye Cleaning: Cleanse the eyes with normal saline or cooled boiled water using a separate sterile swab for each eye.
- Topical Antibiotics: Apply antibiotic eye ointment (e.g., tetracycline or erythromycin) to both eyes. If ointments are unavailable, consider using diluted crystalline penicillin (see dosage instructions below).
Dosage of Diluted Crystalline Penicillin (If Ointments Unavailable – ONLY under direct medical supervision, and ideally as a temporary measure before hospital transfer)
- 100,000 IU vial: Dilute with 4 ml sterile water. Use 5 drops in each eye every 5 minutes for 6 times, then 5 drops every 10 minutes for 6 times, then 5 drops every 30 minutes for 6 times, then 5 drops every hour for 3 days.
- 500,000 IU vial: Dilute with 20 ml sterile water. Adjust dosage proportionately.
- Systemic Antibiotics (with strong caution, only when referral is significantly delayed and under medical supervision): Consider intramuscular crystalline penicillin 50,000 units/kg body weight every 12 hours for 7 days. This should be a last resort and is only acceptable if hospital transfer is delayed and a qualified medical professional has made the decision and is monitoring the infant’s response.
- Referral: Refer the patient to a hospital for definitive diagnosis (gonorrhea testing, culture and sensitivity) and treatment as soon as possible.
Referral Process
- Assessment and Referral: Thoroughly assess the infant’s eyes. Any infant with suspected ophthalmia neonatorum, especially with purulent discharge or corneal involvement, requires immediate referral to a hospital with ophthalmology services. Do not attempt to manage significant cases in a maternity centre.
- Initial Cleaning (before referral): Gently cleanse the eyes with sterile saline or water to remove excess discharge. Use a separate cotton swab for each eye.
Management in Hospital
- Diagnostic Testing: The physician will order an eye swab for culture and sensitivity to identify the causative organism.
- Eye Cleaning: Continue meticulous eye cleaning as previously described.
- Antibiotic Treatment: The physician will prescribe appropriate systemic and topical antibiotics based on the culture results. This may include intravenous antibiotics for severe infections. Penicillin may be used in gonococcal infections, as may other antibiotics like cefotaxime or ceftriaxone.
- Topical Antibiotic Ointments: Use Neomycin or tetracycline eye ointment to prevent eyelid adhesion.
Medical Management Protocol
Purulent discharge in the eyes of the newborn baby → Take history and examine
- Rx for the baby:
- Always wear gloves.
- Cover the inflamed eye with gauze before opening for your protection.
- Clean the eye with saline or water.
- Apply tetracycline eye ointment hourly for 24 hours, then 8-hourly for 10 days.
- PLUS: ○ Ceftriaxone 125 mg IM stat. ○ OR Erythromycin syrup 15 mg/kg body weight 6 hourly x 2/52.
- Rx for the mother:
- Ceftriaxone 250 mg IM stat.
- PLUS: Erythromycin 500 mg for 7 days.
- Rx for partners:
- Ciprofloxacin 500 mg stat.
- Septrin 5 tablets BD x3/7.
- PLUS: ○ Doxycycline 100 mg BD x7/7. ○ OR Tetracycline 500 mg 6×7/7. Educate on compliance:
- Schedule for a return visit.
- Provide mother and partner with condoms and counsel on risk reduction.
Specific Causative Organisms Management
Gonococcal Ophthalmia Neonatorum
- The infant should be isolated for the first 24 hours of treatment.
- Eyes are irrigated every 1-2 hours with sterile isotonic saline until the discharge clears.
- For culture-positive cases or severe infections, systemic antibiotic therapy is indicated. Ceftriaxone (25-50 mg/kg IV or IM) or cefotaxime (100 mg/kg IM or IV) is usually administered as a single dose for localized infection; a 7-day course is recommended for disseminated infection.
Chlamydial Ophthalmia Neonatorum
- Oral erythromycin suspension (40 mg/kg/day divided into four doses) is administered for 14 days.
- Topical treatment alone is insufficient; systemic therapy is essential to prevent systemic spread.
Herpes Simplex Ophthalmia Neonatorum
- The infant requires isolation. Systemic acyclovir (20 mg/kg every 8 hours IV) for two weeks is the standard treatment.
- Topical therapy with 3% vidarabine or 0.1% iododeoxyuridine ointment (five times daily for 10 days) may be added.
- Severe cases necessitate immediate ophthalmological consultation.
Nursing Care Workflow
- General hygiene: Maintain meticulous hygiene, including handwashing, clean linens, and a clean environment.
- Eye care: Continue frequent eye cleaning as previously described.
- Comfort measures: Provide comfort measures to reduce the infant’s discomfort.
- Frequent eye cleaning: Gently cleanse the eyes with sterile saline or water every 2–4 hours, using a separate swab for each eye.
- Medication administration: Administer topical medications as prescribed, ensuring correct dosage and frequency.
- Monitoring: Closely monitor the infant’s response to treatment, including assessment of eyelid swelling, discharge, and corneal clarity.
- Pain management: Provide comfort measures as needed, such as cuddling and soothing techniques.
- Education: Educate the parents on the importance of adherence to the prescribed treatment regimen, proper eye cleaning techniques, and the need for follow-up appointments.
Complications Workflow
Potential Complications
- Corneal ulceration and scarring: This can lead to permanent visual impairment or blindness.
- Perforation of the cornea: A serious complication that requires surgical intervention.
- Endophthalmitis: Infection of the internal structures of the eye.
- Meningitis (rare, but possible, particularly with gonococcal infection): Infection of the membranes surrounding the brain and spinal cord.
- Sepsis: A life-threatening bloodstream infection.
Join Our WhatsApp Groups!
Are you a nursing or midwifery student looking for a space to connect, ask questions, share notes, and learn from peers?
Join our WhatsApp discussion groups today!
Join NowWe are a supportive platform dedicated to empowering student nurses and midwives through quality educational resources, career guidance, and a vibrant community. Join us to connect, learn, and grow in your healthcare journey
Quick Links
Our Courses
Legal / Policies
Get in Touch
(+256) 790 036 252
(+256) 748 324 644
Info@nursesonlinediscussion.com
Kampala ,Uganda
© 2026 Nurses online discussion. All Rights Reserved

