Gynaecology
Genital Prolapse: Rectocele and Cystocele
Table of Contents
Pelvic Organ Prolapse (POP): POP occurs when the muscles and ligaments that support the pelvic organs weaken, allowing these organs to bulge or drop into the vagina.
It is divided into three main categories:
- Anterior Vaginal Wall Prolapse:
• Cystocele: This is the most common type of POP. It happens when the bladder bulges into the vagina. It can be graded from 1 to 3 based on the extent of the bulge:
- Grade 1: Mild, bladder only drops slightly into the vagina.
- Grade 2: Moderate, bladder drops further, reaching the vaginal opening.
- Grade 3: Severe, bladder bulges out through the vaginal opening.
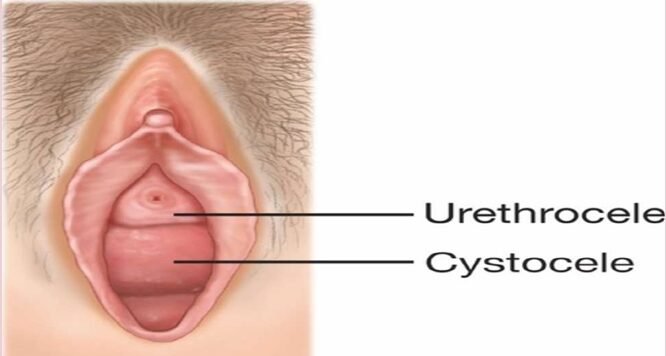
• Urethrocele: This occurs when the urethra, the tube that carries urine from the bladder, bulges into the vagina
2. Posterior Vaginal Wall Prolapse: • Rectocele: This is a bulge of the rectum, the last part of the large intestine, into the back wall of the vagina. • Rectal Prolapse: This is a different condition where part of the rectum turns inside out and protrudes through the anus. This is not a form of POP and is usually mistaken for hemorrhoids.
Prolapse of the Bladder (Cystocele)
Bladder prolapse, or cystocele, occurs when the bladder bulges into the vaginal wall due to weakened supportive tissues.
When both the bladder prolapse (cystocele) and urethra prolapse (urethrocele) occur together, its called Cystourethrocele.
Causes of Cystocele:
- Chronic constipation
- Heavy lifting
- Menopause and decreased estrogen levels
- Pregnancy and childbirth
- Aging / Menopause
- Hysterectomy
- Genetics
- Obesity
- Iatrogenic: Complicated operative deliveries and previous pelvic floor repair operations may be a contributory factor i.e. hysterectomy.
- Pelvic organ cancers e.g. cervical cancer e.t.c
Symptoms of Cystocele:
- Feeling of fullness or pressure in the pelvis
- Urinary incontinence or retention
- Frequent urinary tract infections
- Difficulty emptying the bladder
- A vaginal bulge
- The feeling that something is falling out of the vagina
- The sensation of pelvic heaviness or fullness
- Difficulty starting a urine stream and A feeling that you haven’t completely emptied your bladder after urinating plus Frequent or urgent urination
STAGES OF BLADDER PROLAPSE
- Grade 1 (mild): Only a small portion of the bladder drops into the vagina.
- Grade 2 (moderate): The bladder drops enough to be able to reach the opening of the vagina.
- Grade 3 (severe): The bladder protrudes from the body through the vaginal opening.
- Grade 4 (complete): The entire bladder protrudes completely outside the vagina
Diagnosis of Cystocele:
Initial Assessment:
Pelvic Examination: This helps to examine the vagina and cervix to look for any bulging or prolapse. Assess the size and location of the prolapse to determine its severity. • Abdominal Examination: This helps rule out any abdominal or pelvic masses that might be contributing to the prolapse by pushing down on the pelvic organs.
Further Diagnostic Tests:
- Urinalysis: A urine test can identify any urinary tract infections that could be contributing to bladder symptoms.
- Voiding Cystourethrogram (VCUG): This test involves filling the bladder with contrast dye and taking X-rays as the patient urinates. VCUG can help visualize the bladder and urethra, identifying any abnormalities like prolapse, narrowing, or leaks.
- Cystoscopy: This procedure involves inserting a thin, flexible scope with a camera into the urethra and bladder. It allows the doctor to visualize the inside of the bladder and urethra, looking for any structural problems or blockages.
Imaging Tests (May be used to confirm diagnosis and plan treatment):
• CT Scan of the Pelvis: This scan provides detailed images of the pelvic organs and surrounding structures, helping to underpin the extent of the prolapse.
• Ultrasound of the Pelvis: This non-invasive imaging technique uses sound waves to create pictures of the pelvic organs, aiding in the assessment of prolapse and potential causes.
• MRI Scan of the Pelvis: MRI provides very detailed images, allowing for a thorough examination of the pelvic floor muscles and ligaments.
Evaluating Associated Conditions: • Stress Incontinence Test: To assess whether the cystocele is causing urinary leakage, the doctor may ask the patient to cough with a full bladder. This helps determine if the bladder leaks during increased pressure on the pelvic floor.
Treatment of a Cystocele:
Mild Cases (Grade 1): These often don’t require medical or surgical intervention. Lifestyle changes can help alleviate symptoms:
○ Weight Loss: If overweight or obese, shedding extra pounds can reduce strain on the pelvic floor.
○ Avoiding Heavy Lifting: Limit activities that put pressure on the pelvic floor.
○ Treating Constipation: Regular bowel movements are important to avoid straining.
More Severe Cases (Grades 2-3): If symptoms significantly impact daily life, treatment options include:
○ Pelvic Floor Exercises (Kegels): Strengthening these muscles can improve support for the pelvic organs.
○ Hormone Treatment (Estrogen Replacement Therapy): This can improve tissue elasticity and support in some women. ○
Vaginal Pessaries: These are removable devices that fit inside the vagina to support the prolapsed organs.
○ Surgery: This is considered for significant prolapses or those not responding to other treatments. Surgical options include repairs of the pelvic floor muscles and ligaments, or in rare cases, Colpocleisis (a procedure that permanently reduces the size of the vagina).
Preventing a Cystocele:
- Regular Pelvic Floor Exercises: Strengthening these muscles daily can help prevent prolapse.
- Avoiding Heavy Lifting: Reduce strain on the pelvic floor by limiting activities that require heavy lifting.
- Maintain a Healthy Weight: Being overweight or obese puts extra stress on the pelvic floor.
- Regular Bowel Movements: Prevent constipation and straining by consuming enough fiber and staying hydrated.
- Moderate Exercise: Regular physical activity can help keep the pelvic floor muscles strong and improve overall health.
Join Our WhatsApp Groups!
Are you a nursing or midwifery student looking for a space to connect, ask questions, share notes, and learn from peers?
Join our WhatsApp discussion groups today!
Join NowWe are a supportive platform dedicated to empowering student nurses and midwives through quality educational resources, career guidance, and a vibrant community. Join us to connect, learn, and grow in your healthcare journey
Quick Links
Our Courses
Legal / Policies
Get in Touch
(+256) 790 036 252
(+256) 748 324 644
Info@nursesonlinediscussion.com
Kampala ,Uganda
© 2026 Nurses online discussion. All Rights Reserved

