Tropical Diseases
Tetanus (Lockjaw)
Table of Contents
Definition: Tetanus is a severe, acute bacterial infection characterized by sustained and painful intermittent spasms (twitching) of voluntary muscles. It is commonly known as Lockjaw.
Etiology and Transmission
Causative Agent: The bacterium Clostridium tetani, an anaerobic, spore-forming organism.
Toxin: The bacterium produces the powerful neurotoxin, tetanospasmin, which is responsible for the clinical symptoms.
Source: C. tetani spores are commonly found in soil, dust, and animal feces.
Routes of Entry: Spores enter the body and germinate in anaerobic (low oxygen) conditions, typically through:
Deep penetrating wounds: Puncture wounds, lacerations, burns, and crush injuries.
Umbilical cord: In newborns (neonatal tetanus), infection often arises from an unsterile umbilical cord stump.
Other routes: Ear infections, unsterile wounds sustained during delivery, and septic abortions.
Incubation Period: Ranges from a few days to several weeks, averaging 7–10 days. Shorter incubation periods generally indicate a more severe infection.
Clinical Features
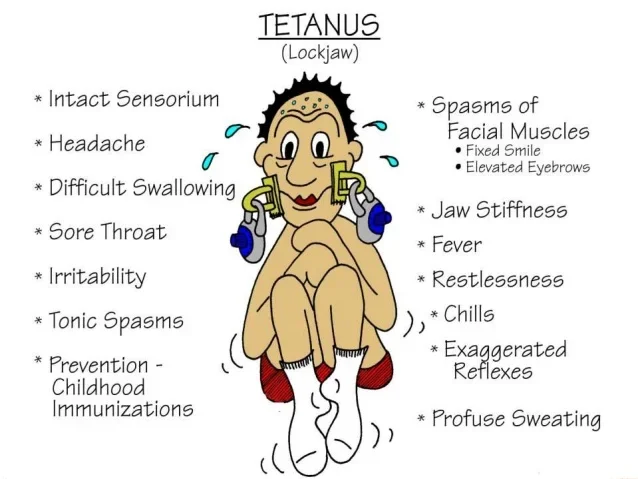
Symptoms usually begin with localized muscle stiffness before progressing to generalized and life-threatening spasms.
Hallmarks of Tetanus
Trismus (Lockjaw): Difficulty opening the mouth due to spasm of the masseter muscles.
Risus Sardonicus: A characteristic fixed, grinning or sardonic grimace caused by facial muscle spasm.
Dysphagia: Difficulty swallowing.
Generalized Muscle Spasms: Severe, painful, and generalized spasms initially affecting the jaw and neck, then spreading to the trunk and limbs. These spasms can be triggered by external stimuli (e.g., sounds, light, touch).
Opisthotonos: Severe arching of the back caused by powerful muscle spasms, while the patient remains conscious.
Other Manifestations
Fever: Often present.
Respiratory Distress: Spasms of the respiratory muscles can lead to respiratory failure, which is a life-threatening complication.
Autonomic Nervous System Instability: Manifestations include fluctuating blood pressure (hypertension or hypotension), profuse sweating, and tachycardia (rapid heart rate).
Hyperreflexia: Exaggerated reflexes.
Absence of a visible wound does not exclude a diagnosis of tetanus, as the entry site may be very small or healed.
Differential Diagnosis
Conditions that may mimic tetanus, requiring careful differentiation:
Meningitis or Meningoencephalitis (Inflammation of the meninges/brain).
Extrapyramidal side effects from certain medications (e.g., Phenothiazine side effects).
Febrile convulsions (seizures associated with high fever in children).
Management
The goals of tetanus management are to relieve symptoms, neutralize circulating toxins, eliminate the source of the bacteria, and control spasms.
1. General Measures and Supportive Care
Referral: Immediate referral to an intensive care unit (ICU) is crucial for severe cases requiring respiratory support (ventilation).
Intensive Nursing: Patients require a quiet, isolated environment to minimize external stimuli that can trigger spasms.
Close Observation: Continuous monitoring of airway patency, temperature, and spasm frequency.
Airway Support: Oxygen therapy and measures to prevent aspiration (careful positioning and suctioning).
Nutrition: Use of a Nasogastric Tube (NGT) for feeding, hydration, and medication administration.
Injection Route: Avoid intramuscular (IM) injections due to risk of bleeding and pain; use alternative routes (NGT, rectal, IV) whenever possible.
2. Neutralizing the Toxin
Tetanus Immunoglobulin (TIG) – Passive Immunity: Administered to neutralize any circulating unbound tetanospasmin toxin.
Dose (Adults/Children): Typically 150 IU/kg IM (administered at least in two different IM sites, separate from the toxoid injection site).
Dose (Neonates): 500 IU IM.
Tetanus Toxoid (TT) or DPT/Td – Active Immunity: The appropriate vaccine must be administered immediately (at a site separate from TIG) to initiate active, long-lasting immunity.
3. Eliminating the Source of Toxin
Wound Management: Thorough cleaning and surgical debridement of the wound to remove necrotic (dead) tissue and eliminate the bacterial spores. This is essential for controlling toxin production.
4. Antibiotic Treatment
First-line: Metronidazole (e.g., 500 mg IV or orally every 8 hours for 7 days).
Second-line: Benzylpenicillin.
5. Control of Muscle Spasms and Pain
First-line Spasm Control: Diazepam (IV or rectal) is the primary agent used to control spasms and muscle rigidity.
Other agents: Magnesium sulfate (can be used alone or with diazepam) or Chlorpromazine. Crucially, patients receiving Diazepam or Magnesium Sulfate require careful monitoring for respiratory depression and loss of reflexes, respectively.
Pain Control: Morphine (IV) or Paracetamol for fever and pain management.
Prevention and Complications
Prevention
Routine Childhood Immunization: All children should receive the recommended tetanus toxoid-containing vaccines (DTP, Tdap, or Td) as per national schedules.
Proper Wound Care: Prompt and appropriate cleaning and debridement of all wounds significantly reduces risk.
Prophylactic TIG: Given to individuals with contaminated wounds and unknown or incomplete immunization status (dose varies by age).
Complications
Respiratory Failure: The most common cause of death, resulting from spasms affecting the muscles of respiration.
Aspiration Pneumonia: Due to swallowing difficulties (dysphagia) and poor airway protection.
Fractures: Severe muscle spasms can cause bone fractures.
Cardiac Arrhythmias: Due to autonomic nervous system instability.
Secondary Infections: Including pressure ulcers (due to immobility) and urinary tract infections (UTIs, often due to catheterization).
Join Our WhatsApp Groups!
Are you a nursing or midwifery student looking for a space to connect, ask questions, share notes, and learn from peers?
Join our WhatsApp discussion groups today!
Join NowWe are a supportive platform dedicated to empowering student nurses and midwives through quality educational resources, career guidance, and a vibrant community. Join us to connect, learn, and grow in your healthcare journey
Quick Links
Our Courses
Legal / Policies
Get in Touch
(+256) 790 036 252
(+256) 748 324 644
Info@nursesonlinediscussion.com
Kampala ,Uganda
© 2026 Nurses online discussion. All Rights Reserved

