Paediatrics II
Pemphigus Neonatorum
Table of Contents
Definition
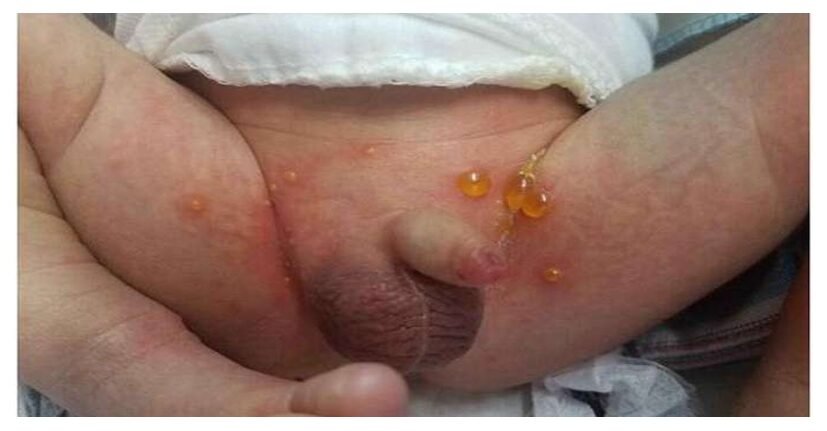
Pemphigus neonatorum is a rare, self-limiting, and usually benign form of pemphigus that affects newborns. It’s characterized by the development of superficial, flaccid bullae (fluid-filled blisters) on the skin and mucous membranes. Unlike other forms of pemphigus, it’s not an autoimmune disease. Instead, it’s caused by the passive transfer of maternal antibodies against staphylococcal exfoliative toxins. These toxins disrupt the desmosomal attachments between epidermal cells, leading to blister formation.
Causes Workflow
Root Mechanism
The root cause lies in the mother’s exposure to bacteria producing exfoliative toxins. These toxins are proteins created by certain strains of Staphylococcus aureus, a common bacterium. These strains carry specific genes (ETA and ETB genes) that enable them to produce these toxins.
Step-by-Step Process
- Maternal Infection: The mother may have a staphylococcal infection, often mild or even asymptomatic (meaning she might not even know she’s infected). This infection could be localized (like a skin infection) or more widespread. The bacteria’s production of exfoliative toxins is the issue.
- Streptococcal from the Midwife if she has a sore throat or septic fingers infected mouth.
- Staphylococcal from a baby if he has septic cord or cut on the skin.
- Antibody Production: The mother’s immune system responds to the presence of the toxins by producing antibodies against them – this is a normal immune response to fight off an infection.
- Transplacental Transfer: These maternal antibodies, specifically those against the exfoliative toxins, cross the placenta and enter the baby’s bloodstream before or during birth.
- Toxins’ Action: The baby now has these maternal antibodies already circulating in their system. Crucially, these antibodies are not directly damaging the baby’s skin. But if the baby is also exposed to the same staphylococcal toxins (either from the mother or the environment), the antibodies can bind to the toxins. This binding interferes with the normal connections between the cells of the baby’s epidermis (the outer layer of skin), leading to blister formation. It’s not the antibodies directly causing damage, but rather their interaction with the exfoliative toxins that disrupts skin cell cohesion.
Clinical Presentations Workflow
Onset and Distribution
- Onset: Typically appears within the first few days of life, sometimes as early as 24 hours or as late as 2 weeks.
- Distribution: Lesions are most commonly found on the abdomen, axillae, groin, and scalp. The face, hands, and feet may also be involved. Oral mucosal involvement is less common than in other pemphigus types.
Bullae Characteristics
- The characteristic feature is the presence of multiple, superficial, flaccid bullae (fluid-filled blisters). These blisters are thin-walled and easily ruptured, leaving a raw, denuded area. The fluid within the blisters is usually clear or slightly yellowish. Nikolsky’s sign (separation of the epidermis with gentle rubbing) is often positive.
Progression and Systemic Symptoms
- Progression: The lesions often heal without scarring within 7–10 days. Healing is typically spontaneous and without residual effects.
- Systemic Symptoms: Usually absent or minimal, although affected newborns may be irritable due to discomfort from the lesions.
Management Workflow
Aims of Management
- The primary aim of management is to provide supportive care, relieve discomfort, and prevent secondary infection. Since the condition is typically self-limiting, treatment focuses on symptomatic management rather than direct targeting of the underlying cause.
- Gentle handling, skin care, wound care, pain management are all supportive.
Maternity Center Management
- Immediate Isolation: Immediately isolate the affected infant to prevent cross-contamination. This involves placing the baby in a separate room or designated area away from other newborns.
- Comprehensive Assessment: Obtain a complete history from the mother, focusing on recent illnesses, potential staphylococcal infections, and the onset and progression of the infant’s lesions. Conduct a thorough physical examination, documenting the extent and severity of the skin lesions.
- Urgent Hospital Transfer: Arrange for urgent transportation of the mother and infant to a hospital with appropriate neonatal care facilities. This is crucial due to the highly contagious nature of the infection and the potential for rapid deterioration.
- Detailed Documentation: Before transfer, thoroughly document all findings (history, examination, and observations) in the baby’s medical record and send this record with the infant to the hospital.
Hospital Management
- Strict Isolation: Upon arrival at the hospital, isolate the infant and all belongings (clothing, bedding) to prevent the spread of infection. Dedicated nursing staff should be assigned to this infant’s care.
- Physician Notification: Immediately notify the attending neonatologist or pediatrician.
- Standard Neonatal Care: Provide standard supportive care, ensuring adequate hydration, nutrition, and thermoregulation. Closely monitor vital signs (temperature, respiratory rate, heart rate).
- Microbiological Testing: Collect a swab sample from a representative lesion for microbiological culture and sensitivity testing to identify the causative organism and guide antibiotic selection.
- Lesion Management: Gently cleanse the lesions using chlorhexidine gluconate (Hibitane) 0.5% or cetrimide 0.5%. Avoid harsh scrubbing. Topical gentian violet 1% may be considered only as directed by the physician.
- Environmental Control: Maintain a dry, warm environment. The infant may be nursed naked in a cot under a radiant warmer to ensure warmth and prevent hypothermia (ensure safe distance and appropriate wattage per hospital protocols).
- Feeding: Continue breastfeeding unless contraindicated. Maintain strict hygiene practices during feeding.
- Continuous Monitoring: Continuously monitor bowel and bladder function, temperature, respiratory rate, and any signs of sepsis (lethargy, poor feeding, increased respiratory rate).
Pharmacotherapy
Antibiotic treatment is considered only in severe cases or if secondary infection is suspected. The choice and dosage of antibiotics depend on the results of the culture and sensitivity testing and the attending physician’s assessment. The following information is provided for context only and should not be interpreted as a prescription.
- Antibiotics (as prescribed by a physician): Cloxacillin or erythromycin may be used. Intravenous soluble penicillin may be administered at a dosage of 50,000 units per kilogram of body weight every 6 hours for 24 hours.
Join Our WhatsApp Groups!
Are you a nursing or midwifery student looking for a space to connect, ask questions, share notes, and learn from peers?
Join our WhatsApp discussion groups today!
Join NowWe are a supportive platform dedicated to empowering student nurses and midwives through quality educational resources, career guidance, and a vibrant community. Join us to connect, learn, and grow in your healthcare journey
Quick Links
Our Courses
Legal / Policies
Get in Touch
(+256) 790 036 252
(+256) 748 324 644
Info@nursesonlinediscussion.com
Kampala ,Uganda
© 2026 Nurses online discussion. All Rights Reserved

